Conditions
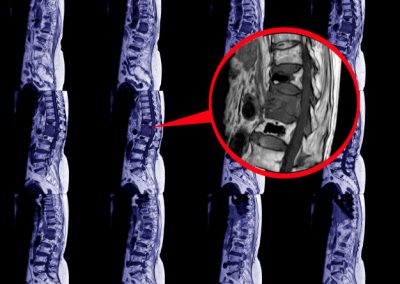
Spinal Compression Fracture
Pain resulting from collapsed vertebrae.
Schedule an AppointmentSpinal Compression Fracture Facts and Information
A spinal compression fracture (also called a “vertebral compression fracture,” or “VCF”) occurs when the bones in your spine, called vertebrae, get so weak that they fracture and collapse. This weakness can be caused by osteoporosis, cancer or benign lesions, and spinal fractures can happen from something as dramatic as a fall, or from simple movements like coughing, sneezing, or turning in bed.
Are Spinal Compression Fractures That Common?
Spinal compression fractures are twice as common as hip fractures and three times more common than breast cancer. Spinal fractures are most common in postmenopausal women over 55.3 In fact, one in two women over age 50 will suffer an osteoporosis-related spinal fracture.
Consequences of Untreated Spinal Compression Fractures
If a spinal compression fracture is left untreated, the vertebra may heal in the “broken” or “caved in” position. This can lead to increased forward curvature, or kyphosis, the medical term for the visible postural change that people refer to as a “dowager’s hump” or “hunchback.”
Just one spinal compression fracture that remains deformed shortens the spine and pushes it forward, adversely affecting spinal alignment. Each additional spinal fracture increases the spinal deformity, and the spinal curvature can become more pronounced. When you change your posture to compensate for kyphotic deformity, it can affect how you walk and can strain your back and joints. A misaligned spine can also compress your internal organs and cause health problems seemingly unrelated to your spine, such as:
- Reduced mobility, loss of balance, and increased risk of falls
- Reduced ability to take care of yourself or perform your usual work or retirement activities
- Reduced days of activity, and more days in bed
- Decreased appetite, and sleep disorders
- Chronic back pain, and fatigue
- Decreased quality of life
- Feelings of isolation and sadness
- Increased risk for future fracture
Diagnosis
- Thorough clinical evaluation. Complete medical history, analysis of your symptoms, and physical examination.
- Testing may include x-rays, MRI and/or CT scans, and electro-diagnosis (EMG). These advanced diagnostic techniques definitively pinpoint the source of pain.
Spinal Compression Fracture Treatment
Disclaimer: the content of the Website is for general informational purposes only and does not constitute advice of any kind. See the full User Agreement here.

Take Back Your Life
Fill out the form or simply give us a call to book your appointment and start feeling better.

Contact Us
Speak with one of our team members right away to get answers to your questions about insurance verification, scheduling an appointment, and our clinic locations.
(732) 955-0655Visiting our Book Appointment page you can instantly request an appointment at any of our Seacoast Spine and Sports Medicine. We offer Free Insurance Verification before your appointment.
Learn how to easily get to the Seacoast Spine and Sports Medicine.
